Your jawbone is the biggest bone in the lower part of your face and it is commonly broken during facial trauma, with only noses getting broken more often.
The lower jaw is medically referred to as the “mandible”, which acts as the foundation for your teeth. Your teeth sit in the “Alveolar bone” which is the top portion of the mandible. This so-called alveolar bone can also be commonly broken during trauma. Depending on the energy and mode of injury that is applied to the face, the teeth and the underlying alveolar bone can fracture, with or without the actual mandible breaking.
On a monthly basis, we are commonly called upon to identify missed injuries in patients that were already seen in the ER (Emergency Room) and Urgent Care Clinics. This all comes down to the training, knowing what to look for. The most common complaint in patients with such injuries is “my teeth just don’t fit together like they used to” or “I cannot close my jaw all the way”. This is because their “occlusion” is off! Occlusion refers to how your teeth come together.
Dr. Massoomi and his team of surgeons in San Francisco, Palo Alto and Cupertino, are trained in the intricate relationship between the mouth, teeth, and facial bones. Oral surgeons are the only field in medicine and dentistry that are trained to reset the “occlusion”, meaning putting back together the important inter-relationships between your teeth and your jaw bone.
Men in their twenties are about 3 times as likely as women to break their jaws. There are a lot of ways the jawbone can be broken, but the most common causes are from motor vehicle accidents, sports injuries, falls, and assaults and so forth. The most common clues or symptoms that something may be off are:
- Pain, swelling, bruising
- Numbness of the lips
- Chipped teeth
- Teeth that do not close properly
- Inability to open their jaw all the way
- Shifting of the jaw to one side when opening
- Trouble speaking
- Trouble chewing
- Trouble swallowing
For many who have experienced facial trauma, the full extent of the injury may not be evident until a few days later. Although for some patients with severe facial trauma, the signs of a fracture appear quickly, in others this is not picked up until sometime later. The case below will demonstrate this.
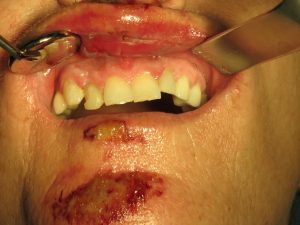
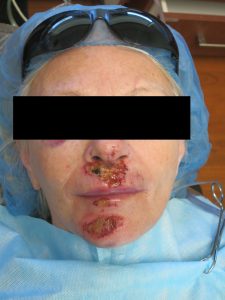 At left is an elderly patient that tripped and fell over the weekend. She was taken to the hospital and to rule-out the most urgent causes, i.e. seizure, stroke, heart arrythemia… Thankfully after ruling out more serious caused for her fall, she was them discharged home on the same day. The following day, the patient started to notice that her teeth were not fitting together, so her daughter called her general dentist, who then called our office for help because they realized that something was off. On presentation obvious signs of trauma are noted based on the bruising.
At left is an elderly patient that tripped and fell over the weekend. She was taken to the hospital and to rule-out the most urgent causes, i.e. seizure, stroke, heart arrythemia… Thankfully after ruling out more serious caused for her fall, she was them discharged home on the same day. The following day, the patient started to notice that her teeth were not fitting together, so her daughter called her general dentist, who then called our office for help because they realized that something was off. On presentation obvious signs of trauma are noted based on the bruising.
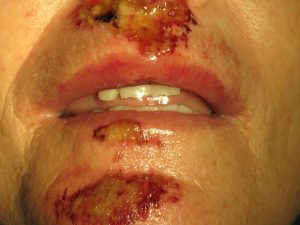 On close inspection her “occlusion” seem to be off, with her front teeth sitting lower than the other teeth:
On close inspection her “occlusion” seem to be off, with her front teeth sitting lower than the other teeth:
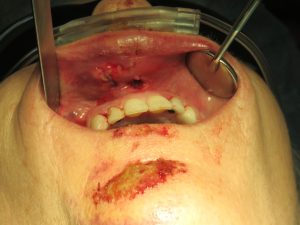
On an intra-oral examination, her teeth present with a “step deformity”, where the 3 front teeth do not line up with the adjacent teeth.
There is an internal laceration that was missed at the hospital. Even though the laceration on the outside of the face was closed with sutures, this was a “through and through” laceration that went from the outside intraorally.
She was immediately brought back to the operating suite, IV sedated in order to “reset” her occlusion and “pop” the alveolar fracture + the teeth back into it original location. The intraoral incision was cleansed and closed with resorbable sutures.
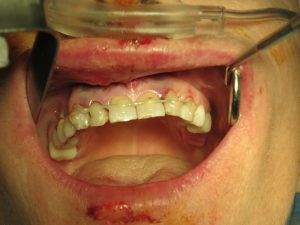
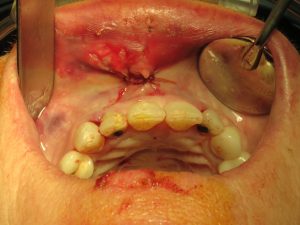 The teeth were bonded together with wire to stabilize them while the alveolar bone and teeth heal for the first 2 months.
The teeth were bonded together with wire to stabilize them while the alveolar bone and teeth heal for the first 2 months.
Above is her one week later, with the teeth and her gingiva, i.e. gums, healthy and pink.
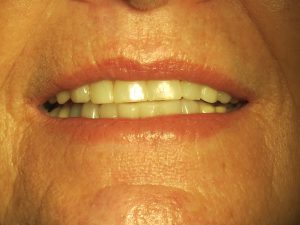
Below is the patient 5 months after the injury:
If you’ve experienced a trauma to the face and notice any of these symptoms, you should seek medical care right away. A trip to the ER (Emergency Room), AND NOT AN URGENT CARE CLINIC, is highly recommended. Most ER’s are better equipped with the right staff and imaging machine (MRI, CT Scans) in order to perform a comprehensive evaluation to rule-out other injuries first, such as concussions and so forth. Once other vital injuries are ruled-out, then the focus will be on the reconstruction of the fractured teeth and jaw bones.
Thankfully surgery is not required in all cases. Dr. Massoomi and his team are Board-Certified in Oral and Maxillofacial surgery will perform a comprehensive examination and do everything possible to put your smile back on your face. If you have had a facial injury and think that your teeth just do not fit together like they used to, call us at 408-358-5000 in downtown San Francisco or 408-253-6084 in Cupertino.